Hospice Providers Penalized for Long-Living Patients
 The federal government is cracking down on hospice companies whose patients live “too long.”
The federal government is cracking down on hospice companies whose patients live “too long.”
Hundreds of hospice providers across the country are facing the catastrophic financial consequence of what would otherwise seem a positive development: their patients are living longer than expected.
Over the last eight years, the refusal of patients to die according to actuarial schedules has led the federal government to demand that hospices exceeding reimbursement limits repay hundreds of millions of dollars to Medicare.
The charges are assessed retrospectively, so in most cases the money has long since been spent on salaries, medicine and supplies. After absorbing huge assessments for several years, often by borrowing at high rates, a number of hospice providers are bracing for a new round that they fear may shut their doors.
[…]
Medicare’s coverage of hospice, which began in 1983, has become one of the fastest growing components of the government’s fastest growing entitlement. Spending nearly tripled from 2000 to 2005, to $8.2 billion, and nearly 40 percent of Medicare recipients now use the service.
To be eligible, patients must be certified by two doctors as having six months or less to live, assuming their illness runs a normal course. They must agree not to bill Medicare for curative procedures related to their diagnosis.
With the taxpayer footing the bill for almost all hospice care, we need a system to ensure that the system isn’t being abused. A statistically based control based on aggregate data is the logical and, really, only imaginable solution. Statistical anomalies are going to occur, though, in individual facilities with a relatively small number of patients.
Obviously, this system creates perverse incentives. It’s far from clear what the alternative is, though.
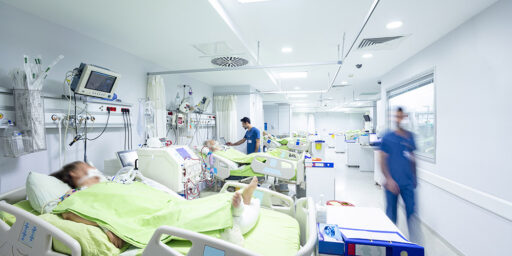
Photo credit: Hospice of Ohio




It seems that the nonreimbursement for curative care would mean that the feds are still saving even when hospice patients live “too long.”
Also, I’m a little suspicious of the regional nature of the problem — MS, AL, and OK? How much of this (if any) is an artifact of CMS’s regional offices auditing different areas by different standards?
Also, the poverty of these areas is probably a factor. People in remote locations with no family support are more likely to need some sort of intervention.
Does this mean that euthanasia will be back in vogue again? Oh wait, that’s illegal. Hmmm… guess they will have to get the Terry Shiavo treatment – let them starve to death when they reach the end of their useful lives.
With so many people thing that “euthanasia” is a teen on holiday in Bejing, I can just imagine that the demand of “death on schedule” is in the offing.