COVID, Age, and Risk Assessment
A vaccinated 75-year-old is as likely to die as an unvaccinated 53-year-old.

In New York’s Intelligencer, David Wallace-Wells tells us that “The Public Continues to Underestimate COVID’s Age Discrimination.” Indeed, while I’ve long understood that the risk of serious complications is next to nonexistent for children and very high for the elderly, I didn’t fully comprehend the extent to which this was—and remains—true. And the issue seems to be one of data visualization.
[I]n assessing an individual’s risk of dying from covid, age appears still as important—and maybe even more important—than vaccination status. And while encouraging further vaccination remains by far the best tool we have in fighting the pandemic to an endgame détente, we should also be clear along the way about the continuing risks to the vaccinated elderly and what might be done to protect them.
Most people know the pandemic has hit the elderly hardest — that is the meaning of the age skew, that the disease grows much more severe the older you are. But if they have seen a chart illustrating this, it probably looks like this gentle upward slope, from the UK’s NHS:
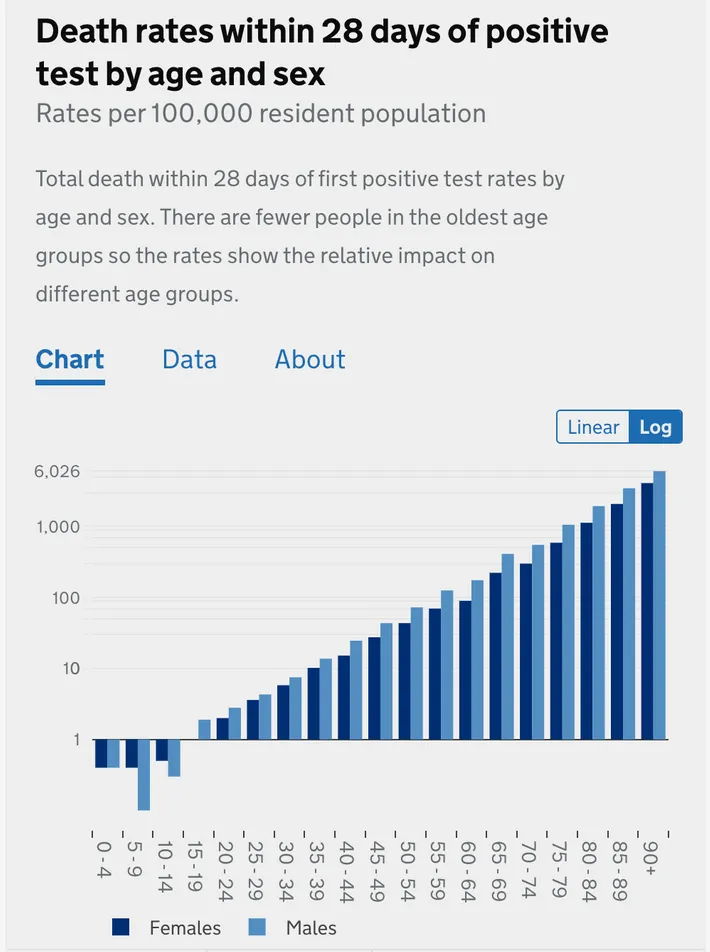
That is a logarithmic chart, which means that the y-axis scales exponentially — a change from one to ten looks to the untrained eye like a change from one to two). That means a huge variation is concealed by presenting mortality risk data in logarithmic form. A chart of the same British information presented linearly (the graphing format you remember from elementary school).
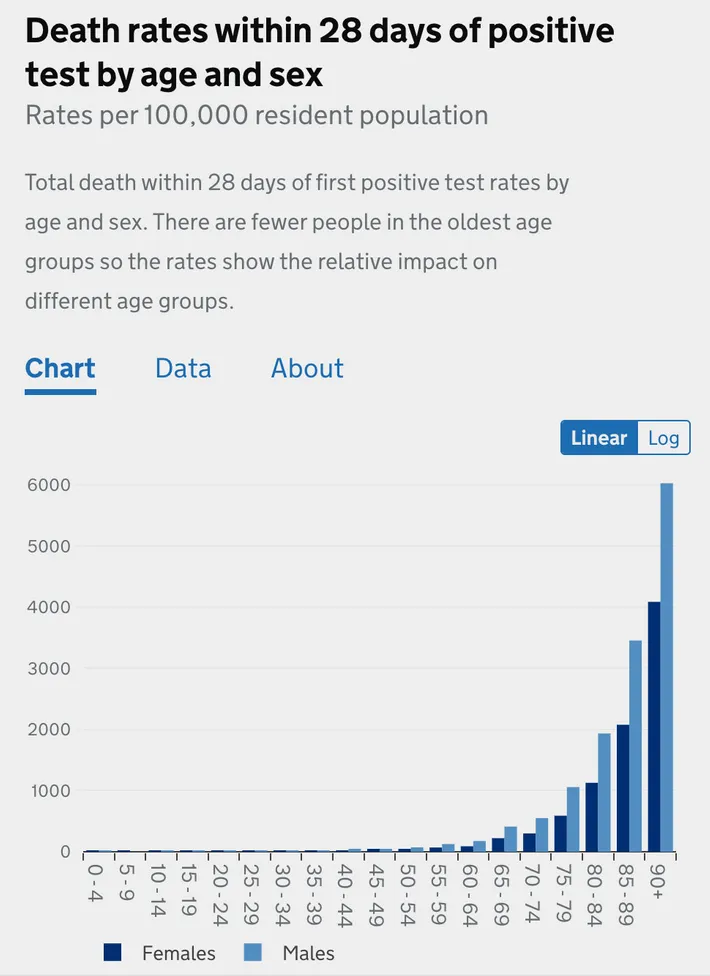
That’s . . . rather more clear!
Why on earth, then, would public health officials and journalists present the data in a way that obscured the real picture in this way?
Viewed this way, the deaths from those under the age of 50 are more or less invisible. To scale the graph to make them visible — which would show that the risk slope from children to 50 year olds is about as dramatic as the slope from 50 year olds to 90 year olds — would require zooming in so close that the bars representing elderly outcomes would tower far above the top of your screen.
So, because most of the data are essentially invisible in the linear format, they’re using a logarithmic scale. But, since most of us aren’t trained to visualize data this way, it actually obscures reality much more than the other way.
After 18 months of public-health guidance promoting universal vigilance, I think hardly any American has a clear view of just how dramatic these differentials are. All else being equal, an unvaccinated 66-year old is about 30 times more likely to die, given a confirmed case, than an unvaccinated 36-year-old, and someone over 85 is over 10,000 times more at risk of dying than a child under 10. And although many infections still go undetected (complicating any attempt at a universal calculation of risk), your chances of dying from a confirmed case roughly double with every five to eight years of age, as countless data across multiple countries demonstrated last year — an effect larger than even the most significant comorbidities. The “exponential growth” of mortality risk by age is, in other words, another aspect of the pandemic we have processed only poorly.
[…]
[F]or all its transformative, liberating power, vaccination has not broken the basic age skew of the disease or offered anyone an exit ramp from it. Instead, in two profound ways, vaccination has confirmed the age skew: by producing severe breakthrough cases concentrated overwhelmingly in the elderly and by reducing the risk faced by individuals by an astonishing degree that is nevertheless smaller than the still more striking effect of age.
There are, of course, quite a number of public policy areas where the average citizen has similar misperceptions. For example, most wildly overestimate how much we allocate to foreign aid. But this issue is one that’s directly tied to individual-level decision-making and behavior.
According to an analysis of British data by the Financial Times, a vaccinated 80-year-old has about the same mortality risk as an unvaccinated 50-year-old, and an unvaccinated 30-year-old has a lower risk than a vaccinated 45-year-old. Even a 42-fold reduction, as was found in King County, would only be the rough equivalent of the difference between an unvaccinated 85-year-old woman and an unvaccinated 50-year-old — the sort of person who was very worried last year before the arrival of vaccines and who may this year be worrying many of those around them by not getting one.
To be clear: They should get one since doing so reduces disease transmission significantly, thereby limiting the future course of the disease, and because it would reduce their own risk of death from COVID by such a dramatic degree that it doesn’t even make sense to call it a degree. But it’s a sign of just how large the age skew is to begin with that getting vaccinated doesn’t deliver you into an entirely new category of pandemic safety — safer and more protected than anyone who hasn’t gotten vaccinated — but simply pushes you down the slope of mortality risk by the equivalent of a few decades.
On the other end of the age spectrum, the same skew is more comforting. Recent data from the U.K. illustrate the phenomenon neatly: unvaccinated children are safer from COVID-19 death than vaccinated adults of any age
According to that data, an unvaccinated 10-year-old, who may look like the very picture of COVID vulnerability heading into the school year, faces a lower mortality risk than a vaccinated 25-year-old, whom we might today regard as close to safe as can be. In England, the incidence of hospitalization among unvaccinated kids was lower than that of those vaccinated aged 18-29, and in recent weeks, the hospitalization rate among kids ages 5 to 14 has been only about one per 100,000. Over the course of the entire pandemic, which has killed more than 135,000 Brits, just one boy and seven girls between the ages of 5 and 9 have died; between the ages of 10 and 14, nine girls and five boys have died. These are all tragedies — and each means many more years of life lost than with a death among the elderly — but they are nevertheless relatively few in number. As schools reopened on the backslope of the U.K.’s Delta surge, there were about seven times as many British kids under age 5 hospitalized with the respiratory disease RSV as there were with COVID.
[…]
This is not to say that unvaccinated children face absolutely no risk from COVID, given that many millions of Americans under the age of 18 have gotten sick, and almost 500 have died, over the course of the pandemic. It’s just that the risk those 73 million minors do face is — relative to the risks faced by their parents and grandparents — very, very small. (As I wrote a few months ago, though a better, clearer first line would have been not “The kids are safe,” full stop, but “The kids are safe, relatively speaking”). Precautions are still worthwhile for the unvaccinated young: regular testing, better ventilation in schools, perhaps mask-wearing, too, when community transmission is high. But it is strange and perhaps unfortunate that in the ongoing, unnecessary, often ugly debate about the vaccines — their efficacy, the risk of breakthroughs, and what additional precautions among the vaccinated may be necessary or advisable — almost invariably the discussions describe two groups, the vaccinated and unvaccinated, as though they occupy two uniform and entirely different spheres of risk. Because while the vaccine culture wars are indeed largely binary, and the future of the pandemic in the U.S. largely a matter of how many unvaccinated will get vaccinated, when we discuss individual risk, it simply doesn’t makes sense to talk about vaccinated 15-year-olds and 95-year-olds in the same breath and unvaccinated 15-year-olds and unvaccinated 95-year-olds in a different breath. In fact, it distorts the picture of the pandemic as a whole when we regard risk as neatly divided by vaccination status. That’s because a vaccinated 95-year-old is still probably over a thousand times more at risk of death, all else being equal, than an unvaccinated 15-year-old. Which means we probably shouldn’t be giving those two groups the same advice about masks or social distancing or boosters.
Emphases mine. He goes further:
[T]o believe that the vaccinated elderly are now perfectly safe, as can be tempting to all of us who are desperate for the unvaccinated to get with the program, is to raise an uncomfortable set of questions about the way we have processed risk by universalizing it. If we want to believe, say, a vaccinated 75-year-old is safe, have we now simply normalized a higher level of individual risk than seemed moral to accept as recently as 12 months ago, given that they may not be any less in danger of dying than an unvaccinated 53-year-old? If we are now debating what we can do, in schools especially, to protect unvaccinated children, who are much safer still, should we not be discussing at the same time what measures can be taken, beyond boosters, to protect the vaccinated elderly? Mask wearing offers differential benefits, too: according to the much-applauded study in Bangladesh, cloth masks of the kind typically worn by children offer very little protection, and the strongest effects of surgical masks were observed among the elderly.
While my skills are decidedly rusty and even out-of-date, I’m a trained data scientist who pays a whole lot more attention to the news than the average citizen. If the statistics here are surprising to me—and they are—then it’s reasonable to believe that most folks have no idea at all.
We are, I think, simply really bad at understanding risk.





Is “mortality” here the chance of dying once you have the disease? If so, comparing vaccinated to unvaccinated on that basis seems really misleading since the chief benefit of the vaccine is that it stops you from getting infected to begin with.
Not much to say except ‘yep’, ‘yep’, ‘yep’. But thought I’d mention that I bet the sentence: …most wildly underestimate how much we spend on foreign aid…. actually is somewhat backwards. Polls I’ve seen indicate that most respondents OVER-estimate foreign aid.
@Stormy Dragon:
The contrary actually, they prevent or ameliorate infection progression to being symptomatic.
The risk of the elderly dying of anything is significantly greater than the risk of death for a 50 yo who has the same injury or illness. This is a truth of life applied to a different causation.
A more meaningful study would be, what is the risk of catching Covid at differing ages and vax status.
@Stormy Dragon: I have been in pretty active text-debate with family for the past week or two, subject: vaccinations, why lagging in Red America. So perhaps I’m overly sensitive. But….
When you say, ‘the chief benefit of the vaccine is that it stops you from getting infected…’ I have to point out that it just obviously isn’t true. Fully vaccinated people have gotten pretty damn sick, to the point of needing high pressure oxygen (several medical folks in family). None recalled a vaccinated person on a ventilator.
Main reason for getting vaccinated has to do with public health. In an 80% vaccinated locale, an infected person would breath on 1/3d the number of non-vaccinated people as the same infected person in a 40% vaccinated place.
One thing that would be helpful is if people learned math when they were kids and didn’t laugh at those who love it when they are older. Maybe even learn a bit now???
@JohnMcC:
The fact the vaccine isn’t a 100% effective doesn’t mean the vaccine doesn’t protect most people from getting infected. Acting like a tiny minority of breakthrough cases invalidate the vaccine entirely is a big anti-vaxxer talking point and it’s sad to see you fell for it.
The mRNA vaccines reduce the risk of infection by 91%:
CDC COVID-19 Study Shows mRNA Vaccines Reduce Risk of Infection by 91 Percent for Fully Vaccinated People
If you do get a breakthrough case, it also makes it less severe, but the biggest benefit is it mostly stops you from getting it all to begin with.
James:
I suspect you would like to edit this: most wildly underestimate
I’m going to comment for I think the first time in almost twenty years of lurking to say:
* thank you for this look at the data – visualization matters!
* mortality is only part of the picture… death is not the only adverse outcome of COVID-19, and we are still learning what the long-term impacts of even mild or asymptomatic cases are on adults, much less on children. I also have to confess to bias… as the parent of an under-12 child, my appetite for risk is still relatively low as regards exposing them to these as-yet poorly understood risks.
https://twitter.com/EricTopol/status/1442673040916058115
I was struck by this: “a vaccinated 95-year-old is still probably over a thousand times more at risk of death, all else being equal, than an unvaccinated 15-year-old. Which means we probably shouldn’t be giving those two groups the same advice about masks or social distancing or boosters.”
I think this is certainly true. But the problem with assertions like this about masks and other mitigation rules is that the reality that we all shouldn’t have to do the exact same things is undercut by the fact that the only way to really make them work is to universally apply them.
To wit: the CDC reasonably told us back in June (ish) that the unvaccinated needed to mask up and the vaccinated didn’t have to. But that only works if the unvaccinated actually behave that way, and they didn’t. As such, the only way to make sure that the ones who really need to mask is to make everybody mask, yes?
@Steven L. Taylor: Yup. And the math says we need to do all the things more and longer than seems “reasonable” because of how that exponential curve works. Got to stomp it when it’s still low, because it’s difficult to impossible to stop once it gets going.
This really belongs in the now-dead partisanship thread, but I’ll stick it here instead:
https://twitter.com/PeterHotez/status/1442798564153995273
https://journals.plos.org/plosbiology/article?id=10.1371/journal.pbio.3001369
I don’t think they actually know how many breakthrough cases there are. I officially tested positive yesterday, and both my kids have had it. There was a large 90th birthday party for a local lady on the 12th of September, and from what I understand, every attendee, vaccinated or not, has since tested positive. Several have had to be life-flighted out, but I don’t know about their individual vaccination status.
It’s problematic, though, because that “proof of vaccination” doesn’t mean a damn thing if breakthrough cases are as high everywhere as they are here.
@charon:
Anti-science!
One reason religious fundamentalists find the GOP so agreeable.
[T]o believe that the vaccinated elderly are now perfectly safe, as can be tempting to all of us who are desperate for the unvaccinated to get with the program, is to raise an uncomfortable set of questions about the way we have processed risk by universalizing it.
There doesn’t seem to be a way not to universalize a response to an epidemic that swept across the globe in a matter of months. Populations are universal. The elderly are not separable in any sane way from the rest of us. And what is being asked–masks, vaccinations–is nothing. The correct response would have been to accept the risk for others without being a selfish, whiny POS, and then go onto to working build around the basics of helping others during Covid.
@JohnMcC: Yes, that’s what I meant.
@Cheryl Rofer: We get twelve years of mathematics in primary and secondary school. That doesn’t mean that we intuitively understand the logarithmic progression depicted in a data visualization that’s usually presented arithmetically.
I’m 75. Vaccination gives me the same odds as a 53 year old? That’s great! If only there were other interventions that could improve my functioning by 22 years.
@James Joyner: The general disdain for math – “Do we really need algebra?” puts it outside what people generally use. It’s one more tool for understanding the world.
Do we really need algebra? Isn’t that where we learn exponentials? Which is another word for “logarithmic progression.” Does anyone learn logarithms any more, with calculators? (That last is a real question. It’s easy to imagine they’ve been tossed from the curriculum.)
And yes, data presentation is utterly horrible. I complained about a Times graph yesterday that was so horrible it was hard to believe it wasn’t an attempt to encourage the Republicans. Maybe it’s horrible because reporters don’t understand math either.
@Steven L. Taylor:
Yes, precisely. I don’t mean to pick on Dr. Joyner, but I believe he had a post up saying that this exact advice was overly cautious and would cause people to eschew vaccination because there was no benefit if everyone was to remain masked. I don’t disagree with that, it’s just the communications pickle we’ve been in for nearly two years now–the people who will listen and heed advice are already the ones adhering to public health rules/suggestions/policy. The ones we need to reach are, by and large, the ones who want it stick it to libs/Biden/”my freedom” and other such nonsense, and are apparently immune to reason.
Risk is about odds and probability, two subjects not commonly taught in high school math.
Here’s a simple illustration:
Suppose you’re forced to play a version of Russian Roulette, in which there are one thousand guns. Two contain a live round in the chamber, while 15 have a blank round, and the other 983 are empty. You’re given a gun and instructed to shoot yourself on the temple with it.
The risk of dying is low, only 0.2%. the risk of injury is much higher (blanks don’t have a bullet, but they do fire hot gasses and powder) at 1.5%. The odds of not suffering any negative consequences is 98.3%.
If you think that’s a small risk, ask yourself whether your risk of death within the next five minutes is higher or lower than 0.2%, ditto your risk of injury.
To make matters worse, suppose in this game you go along with 999 other people, each gets a gun handed randomly. You know 2 people are going to die and 15 will be injured. Does that still look good, even if all of you have the same odds of death and injury?
Finally, suppose you are required to take part in this game several times a day for weeks. How does the risk look now?
One thing we have learned for sure from this epidemic is that very few people understand what “exponential” means. Innumeracy is widespread. I have in these threads joked half seriously that innumeracy is a prerequisite for conservatism. Being more precise, well less than half. @Cheryl Rofer: Also for journalists.
The NHS would seem blameless as there’s a button to switch from log to linear. And they’re not to blame for any confusion about overall rates versus case rates. Or for looking at death as the only negative outcome
But stressing the age related risk I fear can, does, lead to inappropriate behavior. IIRC Sweden set out to isolate us olds and let everyone else go. Didn’t work well. In a decent society young people would decide to mask and get vaxxed to protect the vulnerable. But the common reaction is, “I’m gonna partee!”
@Jen:
And they get more and more resistant to reason as time goes on. It’s become a reflex reaction NOT to do what the “libs” tell you to do.
@Cheryl Rofer:
I can say I’ve never needed algebra in my whole life, except for short periods in high school where there were math classes and tests.
That said, math tends to be taught in isolation, as something abstract you need to learn because some authority says so. This is especially bad when results are measured almost entirely by solving abstract equations or problems. I recall many classmates who did brilliantly at tests, and had no idea what a variable is.
I had one semester of probability and statistics, which is probably what has come most handy later in life (along perhaps with basic arithmetic), even if I’ve forgotten a great deal of it.
@Cheryl Rofer:
@James Joyner:
An admission, I was a horrible math student, mostly due to dyslexia. But the problem that @cheryl is getting at, isn’t that math isn’t taught and absorbed, it is that applying the math is glossed over. I’ve convinced that some of the math teachers that I had could go through the equations, but couldn’t apply them in real life as @Kathy: points out.
It wasn’t till I got to grad school and needed to fulfill a prerequisite of a course in applied statistics that I began to understand why the pain of learning math was worthwhile.
Oh, good. It is nice to see the media and those who look to the media for their information is catching up with what was obvious by June of 2020. Perhaps the mass delusion is waning and those with pundit platforms will face reality. Ron Desantis saw this early on and protected his elderly population in Florida thus avoiding the mass casualties like Andrew Cuomo, Gretchen Whitmer, etc. did where they seeded nursing homes with cases.
A big part of the problem is that those in control of the pandemic response are themselves very old and, thus vulnerable to the virus. Anthony Fauci, Joe Biden, Nancy Pelosi, Chuck Schumer, Mitch McConnell, etc. are all in high risk demographic. Throw in the obese, which is the second highest risk factor and you see those making decisions may not be making them with logic but rather with their personal fear. It got sparked by the fact that the early cases were “special” people with connections. A large percentage of the early super-spreader events were “society” events, funerals, retirement parties, etc. in which a world-traveller jetted in to see and be seen. Unfortunately, they also spread the virus to the service staff.
There are a few issues with the way that math is taught that contribute to its treatment as an abstraction.
One, the way it’s taught seems to be difficult for some. (I include myself in this group.) I received middling grades in most math classes because it felt dull to me–with the exception of my Advanced Math class in high school. This was during my senior year and the only real difference was that my math teacher just seemed to go about teaching math in a way that was not just interesting but more understandable to me. It was ridiculous that my best grades were in the most difficult math class I’d been in, and the only thing I can think of that made it so was the teacher.
There’s also the issue of connecting the need for numeracy to “daily life.” I use fractions almost every day–why? Because I cook and bake. There are two of us in this household, so I frequently scale recipes up and down. Budgets, savings, interest rates/rates of return, measuring rooms for furniture placement, scale, the amount of paint needed to cover a room, how much farther I can go on a 1/2 tank of gas–math is EVERYWHERE.
Rather pathetically, math became politicized during the whole outcomes based education/common core kerfuffle. I am going to lose my dang mind if another friend posts some stupid meme about how they find common core to be nonsensical. If by teaching math a different way we get more kids to understand math and think in a way that makes coding understandable, that’s a good thing. I don’t really care if it’s different–in fact, that might be the saving grace.
Finally, we need to do better teaching logic as well.
@Cheryl Rofer:
One of the biggest issue with the initial pandemic pandemic response was the simple fact that most people don’t understand “exponential”. They just don’t.
Here’s a very simple way to test your friends.
You own a one acre lake. There is one lily pad in the lake. The lily pad doubles in size every day. The lake will be completely covered in 30 days. How many days will it take to cover the lake 50%?
Most people, MOST, won’t give the correct answer of 29 days.
Why? Because they don’t understand/know exponential growth.
The pandemic was a perfect of exponential growth, but people were too stupid to know it.
500 dead minors is nothing to sneeze at. The amount of resources we spend to even avoid an unnecessary death of a single child is staggering – think dead polio vaccines, playground safety, baby seats, etc. Without vaccines, and I mean vaccines for all, that number would surely be in the thousands. So yes vaccines do serve a dual purpose, save oneself and save others. I don’t think viewing fatality rates the way the chart shows accounts for this. More to the point, the opportunity cost of the vaccine is almost infinite, there is really no reason not to take it if you can.
@Raoul:
1254 children under the age of 18 died in the US in the Swine flu epidemic of 2009 in a 12 month period. But the old were essentially unaffected, more likely to die of the seasonal flu that year. So the old people in positions of power didn’t panic because they weren’t at risk.
@JKB:
Citation, please. IIRC, one of the initial superspreader events in Boston was a biotech conference, not a “society event.”
The initial waves of the virus presented issues for densely-packed places, so cities were at greater risk.
DeSantis has been atrocious. There have been over 54K deaths in Florida alone, and that number is likely under-reported.
@JKB:
Florida has as many Covid deaths as New York, and these deaths have happened long after Covid arrived. New York was hit at the beginning when nobody wanted to believe Covid was as bad as it was, and then clamped down. Florida and DeSantis let this happen, and sycophants like you have cheered it on.
@JKB: According to academic.oup.com 317 children died in the US due to the swine flu of 2009. I cannot vouch for the site and I know fatality estimates were raised at a later date (age distribution unknown). Nevertheless, you do have somewhat of a point which I don’t think is well articulated.
@Jen:
I wouldn’t say “large percentage”, but there were a number of SSEs in the extended New York City metro area that were religious: weddings, funerals, religious leader special birthday, etc. Probably fewer than it seems, because the major media in the NYC area did so much coverage.
There’s at least one PhD dissertation out there for some epidemiologist in the future taking what we will then know about the coronavirus transmission and working backwards from the death and hospitalization numbers in 2020 to estimate the “effective” contact rates. I’d bet that there were lots more contact than people were willing to admit.
@JKB:
I’m very pleased to see that you’re still hard at work trying to kill Republicans. Well done.
Oh, BTW, the Arizona audit confirmed Biden’s win, and yet that very night Trump said he won the audit. My interest in abnormal psychology impels me to ask: how do you parse that?
And given that the audit found an over-count of Trump voters, don’t you think we’d better hunt down those election cheaters?
@Michael Cain:
People were taking the subway without masks, working in sealed-off office buildings, and hanging out in crowded bars and restaurants up until the first week of March in NYC. I went to see a show in late February at Brooklyn Steel which was densely packed and I remember thinking about Covid in Italy and being like well, this may be my last outing for some time. Basically, the entire city was an SSE until everything shut down.
@JKB:
When you watch Logan’s Run, who do you root for?
Anyway, deaths in Florida have not born out the “DeSantis did it right” story. Take a look at the graphs in yesterday’s post, where the deaths in red states are way higher.
@Jen: I think the “world-traveler” who “jetted-in” might just be code for “globalist”.
@Stormy Dragon: Understood. Completely understood! Can’t tell you how glad I was to get my shots.
But the expectation of 100% protection is not met by any vaccine. And the reason we count on, for example, the MMR to protect from measles & mumps is because of the widespread nature of the mostly-protected.
@Kathy: I use algebra all the time in practicing law. It is all about constants and variables. “If you go to trial, there is X chance you will be found guilty, and then a Y chance you will go to prison for Z years.”.
@Cheryl Rofer:
I’m decidedly pro-math but, yes, I see a lot of this. Most of the “Do we really need algebra?” debate, as I understand it, is practical rather than disdainful. That is: A whole lot of people simply seem ill-equipped to learn it and, if passing algebra is a prerequisite for high school graduation or getting into college, a lot of people are simply going to be left behind.
@Cheryl Rofer:
No power on earth would make me math proficient. I’m not glib, it just is what it is. OTOH I can write 800-1000 published pages of fiction in any given year, and do it for 33 years. 40 if I don’t drop dead too soon. Specialization is generally seen as improving efficiency, n’est ce pas? I am a specialist and very efficient. Would it be cool to know more math? Sure. But I also want to know more history, art, architecture, biology. . . and all that sort of knowledge acts to improve my efficiency, while laboring over algebra does not.
@Jen:
Not exactly. I argued that the way to get people to vaccinate is to make it a gateway to something like a “normal” life. No, my immediate reaction when the CDC issued its “No Mask Required If Vaccinated” guideline was that, without some enforcement via a vaccine passport or such, the unvaxxed would free-ride to the detriment of my 10-year-old, who can’t get vaxxed. Which I why I was arguing for vaccine passports almost immediately after vaccines started rolling out.
What all these numbers and stats mean, is that even after vaccination we should keep up other precautions like distancing, masking, hygiene, etc., until case numbers go way down. I’ve been saying this since vaccination started last year.
A COVID vaccine right now is different from a measles or polio vaccine, because SARS-CoV-2 is in wide circulation because we’re in the midst of a global pandemic. Polio is still out there, but it doesn’t circulate globally in anywhere close to the same extent.
I look at “95% effective in preventing symptomatic disease” more like an event thing. That is, every time you risk exposure to SARS-CoV-2, which is to say any time you’re close to someone else, you have a 5% chance of being infected and developing symptomatic disease. therefore, it makes sense to see the two doses of Pfizer as an additional layer of protection, rather than as a stand alone, all-protective aegis.
I don’t know if that’s the view clinicians and epidemiologist have or not, but it’s the one I find most sensible.
@Raoul:
Here are the numbers that JKB is citing:
https://www.cdc.gov/h1n1flu/estimates/april_march_13.htm
FWIW, because of motivated thinking, he seems to miss that the elderly death toll is still higher (or at least equivilent) than those 17 and under:
Once again, @JKB never lets the details get in the way of his narrative.
@mattbernius:
Above, first number is the midline estimate, and the range is the estimated low to high projections (which are estimates to include cases that were most likely H1N1 but were not tested to confirm).
Also note a significantly higher high end for elderly than with under 17’s.
@EddieInCA: One of the tricks in that particular problem is that most people don’t realize that you can go backwards from the final answer, too. When I’ve reminded students of that feature, most get the answer right away.
@JKB: “1254 children under the age of 18 died in the US in the Swine flu epidemic of 2009 in a 12 month period. But the old were essentially unaffected, more likely to die of the seasonal flu that year. So the old people in positions of power didn’t panic because they weren’t at risk.”
I worked in a hospital at the time, and they were worried.
And the right was howling at Obama.
@James Joyner: I’ve noted many times in the past that significant numbers of tasks are not “hard” as much as they are “labor intensive.” Language learning, writing (non-creative type), and math are 3 examples. I wish we would go beyond “some people just can’t learn” math to the more accurate “some people are not interested enough in mastering it in our time frame/at all” so that we could better identify the truly innumerate to change our expectations, but it’s too much to ask, I know.
@James Joyner:
Every time you enter a cell address reference in a spreadsheet that is, effectively, an algebraic variable.
I find these thought astounding, as I feel I routinely think in terms of algebraic variables in everyday life.
@just nutha: In fairness, I should have noted that not being able to master a skill in the established time frame is an additional variable that overlaps with “interested enough.” Sometimes the two are hard to separate, though.
@Kathy: I think you’re close, but not quite right. It’s 5% of the risk of an infection that leads to hospitalization or death, compared to an unvaccinated person with the same exposure.
(With an unknown distribution — some people may be more protected, others less so).
What this means in practice is that exposure and risk are cumulative, so minimizing unnecessary exposure is good.
But, it’s not a 1:20 chance of serious illness each time you go to the grocery store. Actual risk depends on lots of other factors, but is almost certainly less than that.
(For instance, half of those infected show know symptoms, and depending on your age, the risk of serious covid is likely lower (unless you are older than I expect), and then there’s masking, ce tilt, length of exposure, the randomness of super spreaders…)
(Do we still have wacky super spreaders with Delta, or did Delta make everyone a super spreader? Early on they were finding that some people spread the majority)
There also appear to be tipping points with how much exposure. 5 minutes a day is less likely than a single half-hour exposure a week. Probably geometric growth of virus and an initially linear immune response or something like that.
@Kathy:
My early (at home) math lessons were on the odds of filling an inside straight with 5 at the table.
@JKB:
Dude, “Grandma needs to die to save the economy” is so last year.
@flat earth luddite: I never learned the exact odds on those types of computations, but they did sort of teach me “cutout points”–when the odds become too long, we stop counting. It’s a variation on estimation.
@just nutha:
I beg to differ. I learned English well enough to read books and watch movies inside of six months, I’d say fluency took a year past that. I flunked Math I (set theory and algebra)*, as well as Math III (analytic geometry) once each. I had to take both again, and I barely made it.
I admit to not being interested, but I devoted tons of time to both. I had to. It was five hours of classes per week, plus homework and studying for exams (English was two hours a week, no homework and no exams). I also had no problem understanding the theory, what moving coordinates about was for and such, but I couldn’t handle the actual part where I’m supposed to “do the math.”
I also had the same problem in Chemistry II (organic chemistry). Much of the course work was balancing reactions, as though that matters if you don’t intend to study chemical engineering.
*What got me was set theory. Algebra was easy in comparison.
When I hear people dismissing the effectiveness of the vaccine I think of a football fan whose team has just won its game 49-14 saying “what’s the point of even fielding a defense if they are going to allow 14 points?”
@Joe: There’s no doubt they’re effective as far as preventing death. I’m slowly changing my mind on this whole “present your vaccine card and the world is your oyster” thing, though. If I abided by that right now, I could still get on that plane Thursday, Covid positive with very few symptoms, fly to Tennessee, and infect who knows how many people. Lots of people who aren’t me probably are or have done just that. I’m leaning towards “present your vaccine card AND a negative Covid test in the last 48-72 hours” for all travel. I mean, if we really want to get this under control, we’re gonna have to take breakthrough cases among the vaccinated seriously and not downplay that risk, as well. Hell, we could just get rid of the vaccine cards in their entirety if we discover breakthrough cases are the norm and not an outlier.
@Jax: Might you consider Mara Lago, rather than Tennessee? We can get you a Trump hat… maybe he will want to meet with some adoring fans.
@Jax: I don’t disagree with your concern and strategy. My gripe is with those who argue that because any single measure that isn’t airtight we shouldn’t bother with any measures at all.
Early in the pandemic, I signed up for daily notifications from my local public health department. Each day, I get an email listing new Covid cases and deaths. The death list includes not names, but number of people who have died by gender and age decade. I have noticed that the deaths have skewed younger starting this summer, compared to this time last year. Instead of mostly people in their 80s and 90s dying, it’s mostly people in their 50s and 60s, with some in their 40s and 30s. So the current Covid wave, at least where I live, is hitting the not-elderly much harder than it did in the past. (Kids and young adults are still not dying).
However, I think we need to get more information out about long Covid. That is one of my big fears about catching Covid, that people seem to have a 10-30% chance of having lasting symptoms, even sometimes when they only had a mild case of the disease. It’s probably harder to track than metrics such as cases and deaths, since it can take a while before you know that your symptoms are lingering enough to be considered long-haul. But Jen I think has pointed this out often: recovery or death are not the only Covid outcomes.
@Kathy: It certainly would be possible for you to be the sort of outlier that I’m alluding to. Indeed, when it comes to Calculus, I would be inclined to claim outlier status, too, although I neither understand the theory, nor can I do the computations. I’d also note that it is entirely possible that the main reason that I failed so spectacularly was that I missed 4 weeks (of 10 total) of the term out with pneumonia, but no, I fail to get the point of calculus–and dem0nstrated to my teacher that term methods that “made more sense” to me worked to achieve the same type of problem solving goal on one subsequent occasion.
My comment was in response to Dr. Joyner’s comment that “A whole lot of people simply seem ill-equipped to learn it.” That may well be true, but it’s not what I routinely observed in 25 years of teaching and tutoring. I DID see a fair number of students who believed “I’m not good at math” (and other things) because they’d been told that they weren’t so often that they imbedded the message.
A number of years ago, I read a history of the preparation of the army to go to war against the Nazis. At first, the educationists the Department of War called on to do the training complained that the trainees were simply too stupid to train. The Department of War indicated that such an answer was unacceptable, and that the experts were to figure out a solution. And they did–once they corrected for the difference in reading level between the trainees and the training materials. Many of the things that became standard practice in schools as I was growing up started in training WWII soldiers.
Now I don’t give a rat’s ass about algebra (although I probably use some occasionally because I scale recipes to cooking for one person) and don’t know whether it should be a graduation requirement or not. What I do know, however, is that large numbers of students in the sorting bins that we called “school” in my day were told “you’re ill-equipped to do X” because telling them that they were too stupid too learn was easier than figuring out how to do better. The state has declared that algebra is an essential skill (at least partially, IIRC, because industry told them it was–and I would know; I was part of some of those conversations). If that’s the case, “some people are ill-equipped to learn” is just as unacceptable of an answer as it was in late 1941 and early 1942.
@Cheryl Rofer:
In my 80-year old dotage, I’ve decided to rectify one of the (many) deficiencies in my education and learn calculus. To do this, I’ve had to go back and refresh my algebra and trig. There are some really good precalculus instructors on the web who’ve recorded their lectures and posted them on Youtube. I was able to buy the books they use on Ebay, and I’m soldiering through. Logarithms are attended to. The algebra wasn’t that sticky — I was surprised how much I remember. The trig, well…the trig I learned some sixty plus years ago was right-angle trig. But, of course, calculus uses unit circle trig. This unit circle thing was entirely new to me and took some doing get my head around. Once I twigged to it, though, I was struck by how elegant the unit circle approach is.
I got my booster shot yesterday. I hope it work through limits and derivatives…
I got my booster shot yesterday.
@Joe: I’m so frustrated with the whole thing. They kept our schools open with masks last year, very few cases within the school system, which kept everybody else relatively safe. No mask mandate this year, and less than a month into it, the whole damn town is sick and our senior citizens are dropping like flies, even the vaccinated ones are struggling. I never go anywhere, but nobody’s safe if they have a kid in school here, that’s for damn sure. Most people aren’t even getting tested, because they refuse to quarantine themselves OR their kids.
@Gustopher: Ha! Sounds like most of the people of Tennessee deserve it, as well, looking at their case rates.
The good news is I got everything but the concert tickets refunded. So if any of my friends on here want VIP tickets to see The Dead South and Reverend Peyton’s Big Damn Band on Saturday, Oct 2nd, at The Caverns in Pelham, Tennessee, I’ve got some!! 😛
@just nutha:
My problem with math, and some other subjects, was the exact oposite: the assumption from my parents and teachers is that I was lazy and didn’t do the work or pay attention in class. I got no help at all.
@Kathy: Indeed. That’s another face of the sorting bin mentality that I mentioned. And good ol’ Protestant work ethic leading to “God’s Blessing” in your endeavor. And if you’re struggling, that on you, you lazy
censored. Work harder!@Jax: I hope you don’t mind, but I used your earlier post about all the people who went to the birthday party coming down with ‘Rona and needing to be life flighted to the hospital too f’n many miles away as a what not to do example for the kids I had in my classes today. I was relieved to see that they really DID get it and are working to get past their inclinations to be lazy about keeping their masks up. We’re still having 500 cases/week in our county, which in reality means that our twin cities of about 50,000 total are having most of 500 cases/week. (They seem to get that, too. Some days, I look at the kids I see at school–today I was at the alternative high school [with the kids who are ill-equipped to do X]–and think maybe they’re up to fixing what my generation smashed to bits. Today was that kind of a day.)
@Just nutha ignint cracker: I do not mind at all! Anything to keep the grannies and grandpa’s safe! The worst part is that most of them had been vaccinated and were kicking their heels up celebrating Helena’s 90th, after a year of seeing nobody. 🙁
@Just nutha ignint cracker: I wish Wyoming had….any kind of public official willing to call for statewide masking. The Governor kicked it down to local school boards and public health officials….all of whom receive death threats.
Soooo….herd immunity it is. May the odds be ever in our favor.
@Jen:
https://quillette.com/2020/04/23/covid-19-superspreader-events-in-28-countries-critical-patterns-and-lessons/
@JKB:
Oh? I’m struck first by your abject cowardice. It’s neck and neck with your dishonesty. But gutlessness and lies are the Republican Party platform now, and you, a coward and a liar, are their perfect representative.
Once again, death is not the only. benchmark we should be using for COVID-19. Long COVID; serious illness; long-term health impacts like kidney, lung, and brain damage; overwhelmed hospitals. The latter has resulted in people with treatable medical conditions dying. And the reason the death rate for younger people is low is partially because they respond better to medical interventions.
Does anyone know whether the referenced study (or any of the others underlying these numbers) controlled for the viral load of the initial exposure leading to infection? My understanding is that higher viral loads lead to, or are at least correlated with, increased severity of symptoms, and it seems likely that it takes a more significant exposure – i.e., a higher initial viral load – to overcome a vaccinated person’s immune response and result in a breakthrough infection. If that’s correct, then comparing breakthrough infections of vaccinated people and ordinary infections of unvaccinated people may not be an apples-to-apples comparison.
In other words, is this really just saying that “a vaccinated 80-year-old [who is exposed to a much higher viral load sufficient to overcome vaccine-induced immune response] has about the same mortality risk as an unvaccinated 50-year-old [who is exposed to a much lower viral load]? If so, it’s not quite as worrisome, or even a particularly surprising, finding.