The Politics of Vaccination
The science and ethics are not the hardest part of determining who should go first.
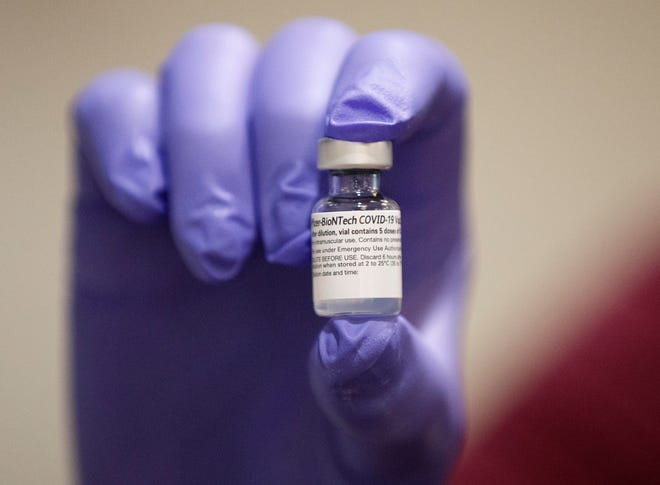
Despite months of President Trump and others downplaying the severity of COVID-19, there is more demand for the new vaccines than there is supply. Naturally, this has sparked a bitter fight over who deserves to get them first.
NYT (“Frontline Workers and People Over 74 Should Get Shots Next, C.D.C. Panel Says“):
Striking a compromise between two high-risk population groups, a panel advising the Centers for Disease Control and Prevention voted Sunday to recommend that people age 75 and older be next in line to receive the coronavirus vaccine in the United States, along with about 30 million “frontline essential workers,” such as emergency responders, teachers and grocery store employees.
[…]
The panel of doctors and public health experts had previously indicated it would recommend a much broader group of Americans defined as essential workers — about 90 million people with jobs designated by a division of the Department of Homeland Security as critical to keeping society functioning — as the next priority population, and that older people who live independently should come later.
But in hours of discussion on Sunday, conducted remotely, the committee members concluded that given the limited initial supply of vaccine and the higher Covid-19 death rate among older Americans, it made more sense to allow the oldest among them to go next, along with workers whose jobs put them “at substantially higher risk of exposure” to the virus.
[…]
Other types of essential workers, such as construction and restaurant workers, would qualify for a third wave of prioritization under the panel’s recommendations. The committee members acknowledged that they couldn’t determine a timeline for that next group, because they did not know how much demand there would be for the vaccine among the earlier priority groups.
WSJ (“CDC Panel Recommends Covid-19 Vaccines for Front-Line Workers, People Over 75 Next“) adds:
The decision to include the oldest people in the next priority group marks a shift for the ACIP, which last month considered giving priority to essential workers over the oldest generations for vaccines in early 2021. That position was based on the argument that, like health-care workers, essential workers are putting their lives on the line to keep the economy and society going.
In addition, many essential workers are older, have high-risk medical conditions, and are from racial and ethnic groups and lower-income populations that have suffered disproportionately high rates of severe illness, according to the CDC.
But some government officials, health experts and members of the public pushed back, arguing that the nation’s priority should be to protect the oldest Americans.
People 75 years of age and older make up 8% of the population but 25% of hospitalizations and have the highest death rate of all age groups by far, according to the CDC. Their rates of hospitalization have also been climbing more rapidly in recent weeks than other age groups, the agency said.
All of that is simple cost-benefit analysis that scientists are more-or-less equipped to handle. But the politics of this makes prioritization much more challenging. Teachers may be less vulnerable than grocery store workers, for example, but there’s a massive push to get them back in the classroom. Prisoners are among the highest-risk groups in the country but, well, they’re convicted criminals. Moreover, there are serious economic and racial equity issues.
A NYT analsyis by Abby Goodnough and Jan Hoffman from earlier in the month (“The Elderly vs. Essential Workers: Who Should Get the Coronavirus Vaccine First?“) dives into some of that.
With the coronavirus pandemic surging and initial vaccine supplies limited, the United States faces a hard choice: Should the country’s immunization program focus in the early months on the elderly and people with serious medical conditions, who are dying of the virus at the highest rates, or on essential workers, an expansive category encompassing Americans who have borne the greatest risk of infection?
[…]
It’s a question increasingly guided by concerns over the inequities laid bare by the pandemic, from disproportionately high rates of infection and death among poor people and people of color to disparate access to testing, child care and technology for online schooling.
[…]
Ultimately, the choice comes down to whether preventing death or curbing the spread of the virus and returning to some semblance of normalcy is the highest priority. “If your goal is to maximize the preservation of human life, then you would bias the vaccine toward older Americans,” Dr. Scott Gottlieb, the former Food and Drug Administration commissioner, said recently. “If your goal is to reduce the rate of infection, then you would prioritize essential workers. So it depends what impact you’re trying to achieve.”
The trade-off between the two is muddied by the fact that the definition of “essential workers” used by the C.D.C. comprises nearly 70 percent of the American work force, sweeping in not just grocery store clerks and emergency responders, but tugboat operators, exterminators and nuclear energy workers. Some labor economists and public health officials consider the category overbroad and say it should be narrowed to only those who interact in person with the public.
[…]
Historically, the committee relied on scientific evidence to inform its decisions. But now the members are weighing social justice concerns as well, noted Lisa A. Prosser, a professor of health policy and decision sciences at the University of Michigan.
“To me the issue of ethics is very significant, very important for this country,” Dr. Peter Szilagyi, a committee member and a pediatrics professor at the University of California, Los Angeles, said at the time, “and clearly favors the essential worker group because of the high proportion of minority, low-income and low-education workers among essential workers.”
That position runs counter to frameworks proposed by the World Health Organization, the National Academies of Sciences, Engineering, and Medicine, and many countries, which say that reducing deaths should be the unequivocal priority and that older and sicker people should thus go before the workers, a view shared by many in public health and medicine.
[…]
There are about 90 million essential workers nationwide, as defined by a division of the Department of Homeland Security that compiled a roster of jobs that help maintain critical infrastructure during a pandemic. That list is long, and because there won’t be enough doses to reach everyone at first, states are preparing to make tough decisions: Louisiana’s preliminary plan, for example, puts prison guards and food processing workers ahead of teachers and grocery employees. Nevada’s prioritizes education and public transit workers over those in retail and food processing.
[…]
One occupation whose priority is being hotly debated is teaching. The C.D.C. includes educators as essential workers. But not everyone agrees with that designation.
Marc Lipsitch, an infectious-disease epidemiologist at Harvard’s T.H. Chan School of Public Health, argued that teachers should not be included as essential workers, if a central goal of the committee is to reduce health inequities.
“Teachers have middle-class salaries, are very often white, and they have college degrees,” he said. “Of course they should be treated better, but they are not among the most mistreated of workers.”
Elise Gould, a senior economist at the Economic Policy Institute, disagreed. Teachers not only ensure that children don’t fall further behind in their education, she said, but are also critical to the work force at large.
“When you talk about disproportionate impact and you’re concerned about people getting back into the labor force, many are mothers, and they will have a harder time if their children don’t have a reliable place to go,” she said. “And if you think generally about people who have jobs where they can’t telework, they are disproportionately Black and brown. They’ll have more of a challenge when child care is an issue.”
There’s a whole lot more, but you get the idea: the calculations are really difficult and depend on what it is you’re trying to prioritize. And there’s a lot of legitimate interplay with the social justice concerns that the 2008 recession and the current pandemic have highlighted.
And, as a USA Today op-ed by Juleanna Glover (“Don’t cut in line for the COVID vaccine. Elites who do will be named and shamed.“) makes clear, there is some deep-seated anger about the whole process.
The U.S. government is laying out broad guidance for vaccine distribution starting with health care workers (21 million), nursing facilities (3 million), high-risk people and those older than 65 (153 million) and essential workers (87 million). Well over 200 million complete vaccinations would have to be administered before the healthy, wealthy and under-65 clients who can afford high-priced concierge medical care should receive a dose if the U.S. health care delivery system were equitable and just.
For context, I should note that “well over 200 million” is two-thirds of the country. In fact, if her numbers are right, they come out to 264 million, or 80.5 percent of the estimated population. We’re almost certainly defining “high risk” and “essential” too broadly.
There are already rumors of executives seeking special dispensation to have their workers newly designated “essential” in order to cut in line. Any new designations should be carefully examined, and governmental agencies should sequester their decision-making processes from undue political influence. The lives of those who have been risking theirs to care for our sick, work in our drive-thrus and stock our grocery stores and drugstore shelves should come first.
Probably. Although it’s quite possible that, given the crudeness of the Labor Department’s job categories, that a lot of people currently designated “essential” aren’t and vice-versa.
Regardless—and it’s a harder position to hold as the Trump era winds down than it was four years ago—it seems obvious to me that the Federal government, and not states and localities, should make these decisions. We should allocate the vaccine centrally, not based on population equities.






Logistics was always going to be the hard part.
Add lobbying by business and labor groups, the LA Times had an article last week about the wealthy hectoring their concierge physicians to get them vaccinated as soon as possible. With some wealthy offering 5 figure donations to the hospitals that are managing the distribution process, in order to be prioritized.
@Sleeping Dog:
Those people should be lined up and injected with the virus.
Here’s the part where “follow the science” does not answer the questions.
One of my law partners came into my office a week or so ago and wondered aloud whether we would be near the head of the line since we were defined by our state as “essential workers.” I reminded him that when our governor recently said if you can work from home you should, we kept all our employees in the office because we judged that we can work in this space in a responsible, social distanced way. Given that decision, I don’t think we get to push to the head of any line. But it won’t stop wishcasting.
Umh, yeah. The U. S. workforce is about 160 million, so 87 million “essential” is 54% of the total. Just silly. I’m retired and 74. Teachers and grocery clerks and baristas should get vaccinated before I do, but how the heck do they get to 87 million? There needs to be some criteria of exposure on top of “essential”.
And what @Mikey: said. Karen snowflakes.
Like anything else, there is always going to be a balance between straight utilitarianism and human perceptions about what is just or fair. I don’t know where that balance should be in this case, but overall I think the federal guidelines are appropriate and consistent with what a majority of Americans believe is the best course of action – as opposed to the opinions of few activists.
I have no problem with the federal government issuing broad guidelines that states and localities must follow, but the feds simply do not have the information or ability to centralize these decisions. Importantly, “essential” workers are defined by each state (and sometimes by locality) and not the federal government, Each state has its own criteria for what is essential and what is considered an essential worker. These have nothing to do with labor department job categories which should actually be ignored.
And there’s the obvious fact that that the virus is affecting different areas of the country differently and that relevant population distribution is not even across the country. States have health departments for a reason – there isn’t a federal government agency that can replace what they do. Centralized control is neither possible nor desirable.
My wife is a teacher and has been in the classroom since Aug 4th. I would not consider her to be at a high risk since the transmissibility in the schools has been show to be fairly low. I think there are higher priority folks.
There is enough data out there on who is at higher risk to make decisions and it should be done in that order (Elderly, physically poor health, prisoners, lower income, etc.). Even my risk level is fairly low even though I’m 66 because of my socio-economic status. I can wait.
@Andy:
The Ohio vaccine distribution plan (required by CDC by Nov 1) places 75+ yo persons (without significant co-morbidities) 16th in order of priority. Now the CDC seems to advocating that these same persons be placed in 3rd order of priority.
My Ohio physician tells me that his office will be getting vials of vaccine next Monday or Tuesday, however it’s not clear to him which of his patients should receive priority.
And while on this subject, it’s interesting that a state or a hospital will be getting vials tomorrow or next week. But what would be more newsworthy is the number of persons actually getting inoculated each day. Since each inoculated person is required to be documented in State and Federal databases, the media should be reporting the number of inoculations per day just as they are the number of hospitalizations and deaths.
Since the elderly disproportionately require healthcare resources and healthcare workers have been stretched beyond their limits for months, getting the elderly vaccinated ASAP along with healthcare workers feels like the correct decision. All of my healthcare friends already need serious mental health therapy as a result of living through this – they can not take much more and collectively we still need them to.
A too broad definition of essential workers leaves the process way too open to manipulation. There should be a preferably-simple and transparent system. But, of course, that would have required planning, so it’s out of reach.
I’d be in favor of making vaccinations public record, minus names. Age, occupation, and comorbidities. And then let the news organizations identify the cases where we appear to get the ordering wrong so guidelines can be tightened.
My instinct is the elderly, and middle-aged-or-over hospital workers should go first.
Or an incomplete, fudgable-but-transparent point system (fudgable in that we lay out the broad point system, but if there are risk factors outside of the guidelines, your doctor can guess about appropriate points; transparent in that the entire calculation is public). It runs the risk of abuse and doctor shopping, but as soon as we put the vaccine supplies into the hands of anyone we have that risk.
Not that this discrepancy matters. I’ll be 73 in January so I’ll just have to wait.
Reminds me of when I was 20 in November of 1968. Two months shy of legal voting age so I couldn’t cast a ballot in the election. Had to wait till 1972 to vote for George McGovern. By which time the legal voting age had been lowered to 18.
None of this compares to the trauma I experienced as a youth while in Grade School in the 1950s.
The first day back to class after the Christmas and New Years Holidays was always January 3rd, even if it was a Friday.
My birthday…
Republican politicians who for MONTHS ON END downplayed the severity of the virus have already been receiving vaccinations, including, for some baffling reason, Marco Rubio–who is not even 50 yet.
This is probably the clearest example I’ve ever seen of a situation that 100% should be easy to prioritize, but still, it’s being screwed up.
Naming and shaming people who try to bump to the head of the line is fine by me. Absolutely appalling behavior.
@Andy:
Is that the premise, or the conclusion?
We know that the analogous arguments fail for (e.g.) educational standards, civil rights, and whether federal courts should be able to overturn state courts. What is special about public health that makes states both more competent and more equitable than the feds in that arena?
@Gustopher:
The part that many people seem to not grasp (not talking to you here, just inspired by your comments) is that the prioritization needs to be a mix of who is at risk of dying, who is at risk of spreading, and who needs to be safe in order to get the economy going again. The definition of “essential” that applies for that last part is totally different from the usual. Day care workers are much higher priority than truck drivers at the moment; grocery store clerks are much more important than hardware store clerks, who are more important than Hallmark store clerks.
…which is why we’re screwed. There is no politically feasible way to actually impose the best prioritization. Especially if it gets devolved to the individual states to do as they please.
@Gustopher:
Making the vaccines public record is a good idea. That’s how we can keep ridiculing GOP Congressmen, like Graham and Rubio, who downplayed the coronavirus for months as just the flu, yet somehow found themselves at the front of the line for the vaccine.
@DrDaveT:
It’s nonsense, of course, an ideological rather than logical conclusion. States are themselves absurd anachronisms. California has a population greater than Canada. In California we have three (nearly four, keep at it Sacramento) major metro areas. We also have a huge, rural farming economy. So, we can centrally plan for 40 million people in very different situations but not for 330 million? Wyoming has the population of Fresno, but for some reason Fresno can be managed by California, but Wyoming has to do its own thing?
@DrDaveT:
So what was the point of requiring the states to come up with their individual plans?
Question: If a state decided to inoculate taxi drivers before ambulance drivers, what is the federal distribution czar going to do about it? Reduce their “promised” allocations?
I vote for giving the first priority to frontline medical personnel, then persons in strategic support positions for the frontline medical workers, and then the most vulnerable people in some order of vulnerability like obese diabetics ahead of a fairly vigorous oldster like me. I don’t have evening clothes, but I’m prepared to do a Benjamin Guggenheim if necessary. Marco Rubio appears to have chosen the guys who dressed as women on the Titanic as his role model.
@Bob@Youngstown:
Once you give the vaccine to the states, there’s nothing the feds can do to control it, other than threaten after-the-fact legal action against individuals that probably wouldn’t stand up in court anyway.
Mobilizing the Public Health Service, rather than passing the buck, might allow the feds to actually control the vaccination rollout. Putting feds in charge of local vaccination operations (since they simply don’t have the manpower to do it all) would be the first step.
A tweet from Elizabeth Warren came across that basically stated she was advised by Congressional physician? to receive a vaccination not because she was old but rather for government continuity of operations purposes. Which would be the reason (not valid in my opinion) for all of Congress to be in front of the line. I can see Congressional leadership but not run of the mill Congresscritters.
I’m high risk, but hardly essential.
shrug.
@Michael Reynolds:
It has nothing to do with populations. It has to do with an understanding of local logistics and resources. Major metropolitan areas mean large hospitals with lots of staff and resources. Wyoming (and most of fly-over country) is significantly more rural than northern California, and will be dealing with small, spread out clinics. That’s the difference between semis full of vaccine, and an Igloo cooler in the back of someone’s pick-up truck.
The people who are essential in a metropolis (be it NYC or LA) are going to be different than the ones that are essential in small cities or rural areas.
And remember: It wouldn’t be Sacramento doing the central planning, it would be Washington.
In order for DC to centrally decide the proper conditions in every area, they’d be…. wait for it: Relying on information and advice from the states–and then using the states’ resources to distribute and administer the vaccine. So why not just let the states do it without the extra layer of bureaucracy?
@Bob@Youngstown:
So that Trump and Congress couldn’t be blamed if vaccination policy upset constituents? Or am I being too cynical again?
The whole rationale for the lockdowns, masks, driving a million+ US persons into poverty and destroying thousands of small businesses has been to keep the hospitals from being overrun. The majority of COVID cases requiring medical assistance, much less hospitalization or ICU, are those over 70. This is also the group with highest mortality rate of 5% which everyone else has a 99.95% of survival.
If they don’t vaccinate those over 70 first, perhaps concurrently with those healthcare workers actually providing care to COVID patients, then we know the lockdowns, masks, etc. were not because they feared the medical system being overrun, but rather politically motivated.
The most idiotic ideas are having people wear identifying patches (one hopes not of a star-like design) or carry ID cards since all that would do is specify who could enter a high virus contaminated are without PPE and not get sick. Of course, the “experts” are scrambling with the fantasy that you could be vaccinated but breath some virus in and then breath it out again somewhere else without your immune system being involved. But then that is not how it works but don’t tell the professors who get quotes in news articles.
@Gromitt Gunn:
While the elderly do require the biggest share of healthcare resources, it would be better to attack the source of the spread first rather than who is taking it hardest. After all, the elderly aren’t catching it in a vacuum; they’re being exposed by caregivers and family. Inoculate those they come into contact with and their risk of exposure drops significantly. Family can wait to visit; it sucks but hey, every essential front-liner worker that’s inoculated first means *the family’s* exposure is less and means they’re safer to go see Grandma sooner. Also, “vaccinated” doesn’t mean “can’t pass on the virus” or even “won’t get sick”. We’re still going to have to wear masks and distance for a long while so better to catch the 20% spreading the most damage first.
@JKB:
Persons being inoculated are getting a vaccination card. They are being told to copy it, put the original in a safe place, and carry the copy with them. (so they can show their favorite bartender or madam)
@KM: At this time we do not know if the vaccines prevent transmission. At this time, the evidence only says that the vaccines prevent infection.
Since vaccines prevent infection, we need to target the people who have the highest probability of having serious consequences of infection. That means we target front line medical personnel as loss of staff leads to increased deaths due to higher probabilities of overwhelmed medical facilities operating in, and for longer, crisis standards of care and near overload. That means we target older Americans first as they are the most likely to both die and consume significant medical resources.
Until we know for sure that the vaccines block transmission, vaccinating staff at nursing homes won’t provide the same level of consequence reduction at a high evidence base.
@JKB:
Says the schmuck as the medical system is currently being overrun and over 300,ooo are dead. You’ve been wrong from the beginning, like your Orange POTUS God you couldn’t care less about the people being driven into poverty, and you really should shut the hell up.
@DrDaveT:
Lots of reasons:
– The distribution and logistics infrastructure is at the state level. Consequently, federal agencies are not resourced or equipped to do this job and were never intended to micromanage mass vaccine distribution.
– The same is true with information and analysis. Most of what the feds get is just passed up from state health departments and is aggregated. The high-fidelity information necessary for distribution is at the state level.
– Each state is different and has different needs and priorities.
The feds therefore don’t have the data or the ability to determine what is actually a fair allocation other than by providing general guidelines, which is what they are doing and is their appropriate role. Again, centralized control of vaccine distribution is not a function the federal government was ever intended to perform.
Even in the federal government, the distribution of vaccine to federal employees will be managed by the agencies and departments themselves and not dictated or managed by any single entity. Again, the CDC or some other health agency doesn’t have the necessary info or expertise to determine, for example, when, where, and how military personnel should get the vaccine. The DoD knows which personnel should get the vaccine first and how best to distribute it. The same goes with the other departments.
Well, random commenters on blogs may not grasp it, but public health professionals at all levels of government certainly do.
That assumes there is a single, objective “best” prioritization.
That would significantly delay the distribution of the vaccine resulting in more deaths. In reality, if you wanted to bypass the states you’d need to federalize the national guard and that would take a ton of time as well and more dead people. All for what benefit? None that I can see.
Again, public health professionals at all levels of government have been working through these problems for a long time. My view is that we should let them do their job.
@Mu Yixiao:
1. Because a coordinated plan will be more effective than a piecemeal set of uncoordinated plans
2. Because some states are run by a party either clueless or antithetical to epidemiology
3. The same reason we don’t let the states decide what rights black people should have.
@Scott: Images of congresscritters getting the vaccine lowers the amount of resistance that other people will have to getting the vaccine.
Rubio might be an unprincipled little douche nozzle, but it’s not about him, it’s about getting the “it’s a Chinese hoax” people to take it seriously long enough to get vaccinated.
@Mu Yixiao:
Because a lot of states are fucking useless (see Florida, Texas, The Dakotas, etc) and we don’t want to condemn the people living there who didn’t choose fucking useless governance?
We don’t want to tie their hands from the outset, but we need to provide clear guidance and demand transparency, and maybe then tie their hands.
@JKB:
Who do you think benefits from lockdowns and —gasp— masks? Why on earth would mask mandates be politically motivated?
Also, there’s a reasonable argument about whether you want to prioritize vaccinating the people most likely to die or the people most likely to spread.
If you cut the number of infections in half, that has the same net effect as reducing the rate of bad outcomes in half. (Bad outcome here is more than just death, as a lot of people who don’t die are going to be dealing with Covid-issues for decades).
Now toss in exponential growth. And then hard math gets involved. Hard math is not the same thing as politics.
@Mu Yixiao:
First of all, the difference between 40 million and 330 million is a difference only in degree, not in kind. We have as much variation within California as the country does.
Second, we have these things called computers. So it’s ridiculous to imagine that data in Cheyenne can’t be present in a database in DC.
Third, most of logistics of delivery will be managed by FedEx and UPS who know where all the medical facilities are. Some of the logistics will involve the military which is an arm of Washington.
Now let’s look at the needless confusion caused by states. People who work in NYC may live in NY, or NJ or CT, or even PA. So if I work in Manhattan and my home is in New Jersey and my doctor’s in CT, whose rules apply? That’s not a question of local knowledge, that’s just local confusion. What if I live in Charlotte, NC but I prefer the priorities being set over the border in SC?
What if I live in a rural area of Nebraska and my closest medical facilities are in Colorado? What if I’m black and live in a racist state that regularly penalizes me?
If you set rules at the national level, by age and by work, you have consistency and the possibility at least, of fairness. 50 states = 50 opportunities for line-jumpers, 50 opportunities for corruption and incompetence, 50 opportunities for preferential or punitive politics. And then there’s the fact that while DC can print money, states cannot, so people in poorer states may be severely disadvantaged.
@JKB:
Actually, we have no evidence that vaccination prevents people from becoming carriers. It’s just not in the way we studied efficacy in the shortened window. There is reason to believe, based on other vaccines, that the rate of transmission would be lower, but nothing about eliminating it.
Also, 5% aren’t even protected by the vaccine. So that 5%, at the very least, can catch and spread Covid.
@JKB:
You’ve been wrong about absolutely everything Covid related. The sane people here have been right.
By the way, JKB, are you participating in your cult leader’s effort to overthrow the United States government? Are you a traitor?
@Gustopher: I understand the PR value of leaders getting the vaccine, but let’s be clear about the messaging. The safety of the vaccine and the need to prioritize recipients are equally relevant ideas needing to be communicated.
The frontline workers in Phase 1 don’t need convincing to get the vaccine, while the elderly at-risk who are still non-believers haven’t earned special urging to get a shot in the arm if they want to continue to delude themselves that the cost of COVID isn’t worth it.
If it’s about getting enough the “it’s a Chinese hoax” people to take it seriously to reach herd immunity, then the time for Rubio was before Phase 3 or 4.
@Andy:
Skipping over many other things I disagree with on factual bases, what on earth makes you think that leaving the rollout to the states would in any way “let public health officials do their jobs”? We have seen the states dealing with this public health crisis for 10 months now, and “letting public health officials do their jobs” without political or simply inept interference has been no part of it in many places. If you want to let them do their jobs, you should favor putting someone in charge who also wants that.
@Gustopher:
You’re probably too young to remember this, but there was a time when we had a COMMUNIST CONSPIRACY to fluoridate water as a way to cut tooth decay. JKB’s spiritual ancestors were convinced that Lefties were conspiring to poison their vital natural fluid. Why? Because, that’s why! Because, um, um, freedom!
When you’re a paranoid loser with a gun collection the search for an excuse to freak out and shoot people is unending.
@DrDaveT:
Why then were the states required to submit their individual plans, if they were not going to be used.
I’m sitting here looking at the 54 page Ohio Vaccination Plan that was required by the CDC. The plan covers everything from preparedness planning to vaccination documentation, who is going to be authorized to give inoculations and the criteria/qualifications that will be applied to those entities ( pharmacies & clinics as examples) as well as education for those reconstituting vaccine and selection of needle sizes.
As far as I’m aware, there is no federal vaccination documentation database, rather each state / Dept of Health has their own.
@Michael Reynolds: Since the mask mandates, sales of carefully crafted cloth masks have skyrocketed on Etsy. And if you look at who Etsy employees donate to… it’s Democrats.
That’s the connection right there!
We dont have enough information to decide what is the “best” plan to use the limited supply of vaccine. The estimates about the effects by the CDC are just that, their best guesses, and if you look at their guesses there isn’t much difference between the groups they are looking at in terms of lives saved. So I think a lot of this comes down to preferences and best guesses. In the over 75 group the 95% confidence level for efficacy is between -12-100%. IOW the vaccine might actually make people over 75 more likely to catch Covid. Most of us dont believe that, but based upon existing data that is what we know.
OTOH we do know that it works very well in the under 65 group. Absent enough good data to make a definite decision you make your best guess which will probably be influenced by your values and your degree of risk aversion. Do you give it to the very old who are dying a lot, but it may not work for them (there are physiologic reasons why they might not work) or use it in younger groups where you are certain it will work and that group is likely the vector for a lot of disease, but then you dont really know if the vaccine prevents infection or just illness?
Steve
After Trump is removed from being the decision maker in D.C., one of the primary reasons I would like to see someone like Biden put together a team to coordinate with states regarding the vaccine distribution is that I do not want to read stories like the baker refusing to bake a cake for a gay couple. This absolutely could happen, someone who controls the vaccine could decide that certain people do not deserve to get the vaccine, and then they could find a friendly judge/politician to agree that it violates that person’s “religious freedom,” or some other bullshit phrase used to justify this person’s refusal to do their job
I loathe pharmacists who use religion as an excuse not to fill prescriptions such as those for birth control,…such utter bullshit. The funny thing is I know a pharmacist who is gay, imagine if he had the right to refuse filling prescriptions of anyone who was not part of the LGBTQ community.
Anyway, sorry for the thread derailment.
If I lived in the Deep South I would want someone in D.C. calling the shots so it would be all but guaranteed that a local politician did not play favorites when it comes to who gets to be first in line.
Actually, quite a few of them do. I read yesterday of one hospital system administrator who said 50% of his system’s employees were “going to wait” to get the vaccine. (wish I could remember where this was).
@DrDaveT:
You can choose to accept it or not, but the reality is that the states have a primary role in vaccine distribution. Wishing that it were not thus isn’t going to change that fact, especially when done at the 11th hour.
And the federal health agencies have made zero mistakes in this crisis? We still have a lack of sufficient Covid testing in this country which is entirely due to the ineptness of the FDA and other federal agencies who are the central authorities for that. The assumption that centralized federal control would magically make everything better on vaccine distribution (or anything else) or prevent all these hypothetical problems is just that – an assumption.
Furthermore, the idea that we should delay the current vaccine distribution – thereby assuring that more people will die – so the feds can do it instead is the very definition of “inept interference.”
@Bob@Youngstown:
Exactly, each state has a published plan that’s been subjected to scrutiny for at least several weeks (Colorado’s plan – my home state – was published early this month). Instead of substantive criticisms that these plans are defective, there’s a lot of handwaving and unsupported assertions.
It will be clear if states deviate from these plans. There are a lot of interested parties that are watching things carefully. Trying to shoehorn more federal control or authority into the middle of this process is only going to slow down and muck up the process.
@OzarkHillbilly: Texas. Houston:
https://www.npr.org/2020/12/16/947248103/at-houston-hospital-head-of-covid-19-unit-sees-some-staff-wary-of-a-vaccine
@Andy:
States also don’t have funding for this role, so… the federal government is going to have to step up there at least. A pile of covid in South Dakota isn’t just a risk to South Dakota, unless we start forbidding interstate travel.
@JKB:
God, you’re a dumb asshole.
Rather than a pissing contest over which is more superior, it would be nice if state governments and the federal government simply worked together and coordinated their plans so as to help the most people…alas…
@Andy:
Why do you say that? What does the FDA have to do with Covid testing? Covid testing is almost entirely in the hands of the private sector. Almost everything in our healthcare system, with the exception of a significant portion of veterans care, is in the private sector.
I have a Covid testing center a few blocks from me, but it is run by the University of Maryland, Medical Center and its funding comes from the state, not the feds. It’s the same with all the non-commercial testing centers in MD
Curse the lack of the edit button. That comment above should read, “the private sector or the state and local governments.”
@MarkedMan:
they approve the tests.
@MarkedMan:
All diagnostic tests have to be approved by the FDA and they have been reluctant to approve various kinds of tests including rapid-at-home tests. This article from August lays out the problem. I can’t seem to do more than one link here at OTB, but a recent article at Vox which covers the approval for one of these tests (which just happened last week) discusses some of the same issues.
Notably, the FDA didn’t even provide emergency approval guidelines for these types of tests until late July.
Had the FDA done that much earlier, and been more proactive about approving non-laboratory and non-prescription tests, then these tests would have been developed and approved much earlier, and they would have been more available for the winter case surge we’re now experiencing.
@Andy: And they let pretty much anyone sell an antibody test with basically no regulation, leading to really shitty tests.
The FDA did a piss poor job at times, and was trying to get better looking numbers for political reasons. Not as bad as Florida, but bad.
I do think that voting in candidates who are basically opposed to governing does not always lead to good governance though, whatever level they are at. A government run by people who think that government is the problem tends to be a self-fulfilling prophesy.