U.S. Emergency Care Sytem at Breaking Point
A new study finds major problems with emergency room services in the United States.
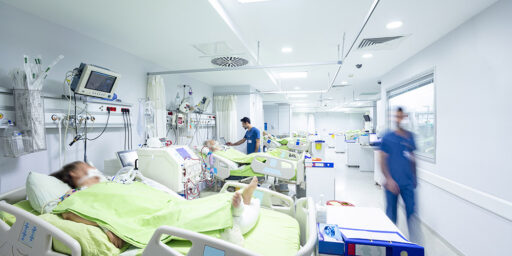
Half a million times a year — about once every minute — an ambulance carrying a sick patient is turned away from a full emergency room and sent to another one farther away. It’s a sobering symptom of how the nation’s emergency-care system is overcrowded and overwhelmed, “at its breaking point,” concludes a major investigation by the influential Institute of Medicine.
That crisis comes from just day-to-day emergencies. Emergency rooms are far from ready to handle the mass casualties that a bird flu epidemic or terrorist strike would bring, the institute warned Wednesday in a three-volume report. “If you can barely get through the night’s 911 calls, how on earth can you handle a disaster?” asked report co-author Dr. Arthur Kellerman, Emory University’s emergency medicine chief.
That ERs are overburdened isn’t new. But the probe by the IOM, an independent scientific group that advises the government, provides an unprecedented look at the scope of the problems — and recommends urgent steps for health organizations and local and federal officials to start fixing it. Topping that list is a call for coordinating care so that ambulances don’t waste potentially lifesaving minutes wandering from hospital to hospital in search of an ER with room. The idea is to set up regionalized systems that manage the flow much like airports direct flight traffic. That also should direct patients not just to the nearest ER but to the one best equipped to treat their particular condition — making sure stroke victims go to stroke centers, for example.
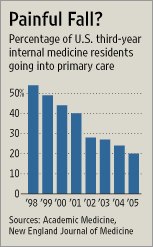
While there are many reasons for these problems, the main one seems to be that the poor and uninsured often rely on ER care for ailments that would send the rest of us to a primary care physician. It’s also the case that ER/trauma care is at the high end of the spectrum for susceptability to malpractice suits and therefore their insurance costs are astronomical. Combined with the fact that a substantial portion of their patients can’t or won’t pay, this is problematic.
Shakespeare’s Sister and Kevin Drum cite this story as proof that the “we have the best healthcare in the world” retort to calls for a state-run medical system is a crock.
Well, maybe. There are certainly huge gaps in our system and the patchwork of part capitalism, part socialism may indeed be worse than either extreme. The fact that someone else pays most of our medical costs takes away any incentive to cut costs, especially when combined with a tort system that further distorts the economics.
Still, one can’t cite a study on problems in one system as proof that one system is preferable to another without demonstrating that said problems don’t exist in the alternative. Is emergency care in, say, the United Kingdom or Canada available in abundant supply without long wait times, overrunning with specialized equipment such as child-sized items, and set up in such a manner that those who need trauma or other specialized care are seldom misdirected?
Apparently, not so much. A study of the Canadian system released last month reveals that “About 85 per cent of emergency room directors working in communities of at least 10,000 people reported a lack of available beds was a major cause of overcrowding” and that “Of the emergency room directors surveyed, 62 per cent called overcrowding a major problem and half thought it posed a risk to patient well-being.” A 2003 study found that they needed major overhaul in order to respond to natural disasters and other crises. A September 2002 CTV report found all manner of problems.
Canadians know there are plenty of problems in Canada’s health care system. But if you want a close-up look at the problems, simply head to your local emergency room. In this CTV exclusive, reporter Avis Favaro found graphic evidence of the chaos in one hospital.
Credit Valley Hospital in Mississauga is just one hospital in crisis. Dr. Eric Letovsky works in the emergency room there, and while he loves his job, he hates what he sees there on a daily basis. On the day our CTV cameras stopped by, five paramedic teams clogged up the ER waiting area, trying to admit sick patients. One woman had a hip fracture, another woman had just suffered a suspected stroke. But there wasn’t a stretcher available to put the patients on.
No one was being admitted. A glance at the board of patient names shows a sea of red names — all the patients waiting for beds upstairs. But most of those patients coming in by ambulance are going to have to wait until another patient can be discharged before they’ll be given a bed. Not only is this emergency room over-capacity, but so are 80 per cent of the hospitals in nearby Toronto. “Basically every hospital from downtown west was not available,” says one of the waiting paramedics.
“This is a normal day,” says Levotsky. “This is a normal day.”
“The provincial and federal governments would like the public to think that everything is good or getting better in the health care system. And it’s really just the opposite,” he says.
A Google search for “UK Hospital Emergency Rooms ” reveals at least anecdotal evidence that they have issues as well.
These stories are all on the first page of results; none of the skipped results provide countervailing data:
Integrated security solution improves hospital security (Paramedic UK, October 2005):
Hospitals have complex security requirements and are faced with a range of threats and risks to patients, staff, expensive equipment and medicines. According a to a report by the Guardian in April 2001, violence in hospitals had become so widespread that for every NHS Trust in the UK, an average of 500 violent incidents during the year 2000.
In almost all major teaching hospitals, police presence has now become routine, especially around hotspots like A&E departments. NHS trusts are also employing their own security guards, hiring private companies to carry out round the clock patrols, using closed circuit TV cameras and alarms, and in some cases giving staff mobile phones and pagers purely for extra security. Staff accommodation has to be protected from intruders, and trusts have had to introduce tight security in maternity units because of the fear of baby snatching. Many hospitals are also plagued by thieves and vandals.Jon Richards of Unison commented at the time: “What is important is to analyse where staff are going to encounter problems. People, who work in mental health, ambulance workers, A&E, maternity units and in the community, are all in the frontline, therefore most at risk”.
Europe diary: Belgian health (BBC, 1 June 2006)
. . . BBC Europe editor Mark Mardell praises Belgian health care, after his son was rushed to hospital . . .
[…]
The hospital is super clean, quiet and calm, in a way that British wards rarely are.
I was rather a fan of the Belgian medical system even before this. I’ve been lucky in having had very good GPs in England and they are equally good here. But it’s easier to get an appointment, even though your phone call goes straight through to the doctor who gives you an appointment herself (or himself). No dragonish receptionists.
The system is based on insurance: the doctor or hospital charges you and you claim the money back off your “mutual”. It’s rather odd that such a system, which frightens the living daylights out of those keenest on preserving free health care in the UK, is used in Belgium and France, which are rather less keen on the glories of free enterprise.
I stress that I write as a consumer, rather witless about my own financial affairs, rather than as a journalist who has studied the system, but the disadvantages are not plain to me, nor do they seem to point to a particular political outcome. What I don’t know is how the mutual system works for someone who hasn’t got enough money to pay the rather large bills in the first place.
An Oxford University Press release for a book published April 2006, Emergency Department Treatment of the Psychiatric Patient: Policy Issues and Legal Requirements:
Many hospital emergency departments are overcrowded and short-staffed, with a limited number of hospital beds. It is increasingly hard for emergency departments and their staff to provide the necessary level of care for medical patients. Caring for people with psychiatric disabilities raises different issues and calls on different skills.
[…]
This eye-opening book explores the structural pressures on emergency departments and identifies the burdens and conflicts that undermine their efforts to provide compassionate care to people in psychiatric crisis. In addition to presenting a new analysis of the source of these problems, Dr Stefan also suggests an array of alternatives to emergency department treatment for people in psychiatric crisis. Moreover, the author proposes standards for treatment of these individuals when they do inevitably end up in a hospital emergency department.
Now, I don’t know how these anecdotes and studies ultimately stack up against the US system. It may be that, despite these problems, they still do ER care better in the aggregate. It’s quite likely that they do it less well for those for whom cost is no object and better for the very poor. Still, let’s not cite every problem in our system as an Aha! moment to prove we’d be better off if only we were more like England or Canada.
UPDATE: From the front page WaPo story on the reports: “Fixing the problems is likely to cost billions of dollars and will require the leadership of a new federal agency, which Congress should create in the next two years, they wrote.” Name the last federal agency created to solve a problem which it then fixed? The Defense Department, maybe?


A nearby city hospital hires and sets doctors up in an offices near the hospital that makes the doctors appear to be in private practice when they are actually on the hospitals payroll. The common practice for these doctors is to work 4 1/2 days per week and it is impossible to contact the doctor during their non working hours. In the event of an emergency or non emergency, these doctors telephone answering machines tell you to go to the hospital emergency room. The doctor in the emergency room will not contact your doctor, even if requested by you, unless it’s almost a life of death situation.
This a dollars and cents issue because these “Hospital Doctors” are only paid for the 4 1/2 days they work.
This might explain why emergency rooms are overcrowded and medical care has “Gone to hell in a hand basket”
Let’s not overlook the number of people who visit ERs for common ailments that don’t really require immediate or expert attention. I’ve sat in the waiting room 3 times in the past year (broken humerus, stitches x 2). Most all patients were there for colds or rashes or minor injuries that would be fine with first aid. Of those who didn’t really need to be there I believe ALL were insured through Medicaid.
Every time I read or hear the words uninsured, I wonder who these people are. I work in the health care system and I don’t know any uninsured people except the self-employed.
L
Gee James, you are such a meanie. Using data and logic to basically poor cold water on Drum’s “Aha! moment”.
As I’ve aregued all along, a socialized health care system might work really well at curtailing costs. After all, increasing wait times can discourage some people from seeing a doctor. If you don’t see a doctor, it can reduce costs at least monetarily. The costs of sitting in a waiting room for an hour then going home to be sick for a longer period of time or even dying isn’t usually captured.
But trying to get Drum or anybody else who favors socialized medicine to pay attention to things like this is impossible. Add on the fact that our health care systems treats as “insurable” things that really shouldn’t be such as pregnancy. A woman can control when she gets pregnant these days. If she gets pregnant she basically chose to do so. Why is that insurable? Who chooses to have a heart attack, a broken leg or get hit by a car? The latter are all unpredictable to a large extent whereas pregnancy is the usual outcome of unprotected sex. A couple has unprotected sex and she gets pregnant…what a Goddamned freaking shock! Who saw that coming?!?!?
So will a socialized health care system cost less? It is possible that the decreased visits to emergency rooms will lower over all costs without adversely impacting health care in general. Might even improve it. However, we also have to consider that visits to primary care doctors will increase, probably by a larger amount than the decrease in emergency room visits. Why? Because the poor and homeless use the ER as the doctor-of-last-resort. This means they usually go only when they absolutely have too. Subsidize visits to primary care docotrs and they’ll likely go much more frequently.
What is the net effect? Beats me, but then again I’m honest. Drum, et. al. will tell you that a panacea awaits at the end of the road of socialize medicine. Bottomline, I think you are right to be skeptical.
“Add on the fact that our health care systems treats as �insurable� things that really shouldn�t be such as pregnancy. A woman can control when she gets pregnant these days. If she gets pregnant she basically chose to do so. Why is that insurable?”
You’re kidding right? This is the most idiotic thing I think I have ever heard. As if pregnancy (a necessity for our continued existence on this planet) should be treated like an elective procedure (such as a nosejob). If someone “chooses” to eat bacon and smoke two packs a day, should insurance pay for his heart attack?
herbavida:
Steve’s point is not that pregnancy is somebody’s “fault” and therefore shouldn’t be covered but rather that it is a routine life event, not an unexpected “illness.”
Automobile insurance does not cover replacing worn tires, batteries, brakes, and similar events; it’s just there for major accidents. Similarly, homeowner’s insurance doesn’t cover painting, lawn care, or replacing an old, leaky roof. By creating the expectation that health insurance covers everything, we certainly make it much more expensive and thus less affordable for those at the bottom of the economic ladder.
My local hospital recently built a deluxe care wing. A beautiful building with a great deal of open space it looks like a grand hotel. It even has special butler service (their word, not mine)for meals and pampering. I guess since the needs of the low income patients and emergency patients were met they could build such a facility, right? No, not really, they built it because a board of directors wanted to attach their names to something large and pretty. Rather than make solid decisions about helping people many boards are just egotistic.
Emergency room upgrades could easily be accomplished with a shift in priorities. I doubt that shift will take place. The glory does not rest in effective health care delivery but in impressive buildings.
Also keep in mind that an advocacy group agitating for more tax dollars produced this “report”. If we believe every document such as this we would have to tax ourselves to death. It’s economics, scarce resources and how to allocate them.
I have yet to see hospitals push for immediate care centers that can stitch up a cut or treat a sinus infection without using the tremendous resources of a typical emergency room. It’s a simple cost effective solution but administrators and boards are not interested.
I find it funny the health care cabal has screwed it up (according to the report anyway) but points to the taxpayers for $$$ to fix it. Physicians heal thy selves.
I see you axed my post. [truncated]
Editor’s note: Learn to have rational, adult conversations. If you direct abusive comments toward writers on the blog, they’ll be deleted. Do it often enough, you’ll be banned from the site. Dissenting views are welcome; insults are not.
I’ll repost my previous post, since it seems to have disappeared:
James,
I think Steve’s point is quite clear–he views pregnancy as “elective” or “avoidable” and should therefore not be covered by insurance. Again, many heart attacks are “avoidable”–should they be covered?
[*********] Pregnancy is a “routine life event” but it also carries health risks to both mother and child and MUST be covered by health insurance. Denying health insurance to pregnant women results in unnecessary (and avoidable) illness and death. It is that simple. BTW –are you pro-life?
[*********] Access to comprehensive health insurance (unlike car insurance or homeowners insurance) has life and death consequences. Health insurance does and SHOULD cover the “maintenance” of the human body, and not just emergencies. One surely “chooses” to have a yearly check-up, but those yearly check ups help avoid emergent health problems that are MUCH more expensive to fix after the person gets sick.
Also, health insurance does not cover “everything”. Usually it does not cover elective procedures (like plastic surgery ) as I mentioned before. You are building a straw man when you say there is an “expectation that insurance cover everything”. There is no such expectation. People are fully aware that they cannot get breast implants if they are on medicare. They do and should expect to receive coverage for medication and treatment that enable them to AVOID expensive acute illnesses, complications, injuries or death. Including coverage for pregnancy.
[*********]
[Editor’s note: Abusive comments deleted with attempts at rational discussion remaining as an illustration.]
herbavida:
I don’t contend that care for pregnancy isn’t beneficial. Indeed, so is putting servicable tires on a car. The latter, however, is not covered by “insurance” because it’s considered a routine expense and not a “risk.”
My preference is to cover pregnancy and even routine checkups. Doing so might even hold down lifetime costs.
Still, Steve’s point that including those things substantially increases the costs of insurance–and, thus, serves as a barrier to entry for those at the bottom–is certainly true. It may be that there should be policies that cheaper and cover only catastrophic illnesses and others that are more expensive/inclusive.
“Still, Steve�s point that including those things substantially increases the costs of insurance�and, thus, serves as a barrier to entry for those at the bottom�is certainly true. It may be that there should be policies that cheaper and cover only catastrophic illnesses and others that are more expensive/inclusive.”
Wrong, routine care has been proven again and again to LOWER overall healthcare costs. Check-ups and routine health care is MUCH cheaper than expensive procedures and treatments of serious diseases/conditions/complications that could have been avoided by routine health care.
http://hffo.cuna.org/story.html?doc_id=982&sub_id=12433
Clearly there is a serious problem here. What we need is a lot more articles about how the Canadian & French health care systems are on the verge of collapse. That should do the trick…
The lowest cost way to provide a service is to limit the surge capacity because surge capacity is idle capacity.
Thus your telephone system is designed to handle Mothers Day. It overloads on 9/11 type events.
The cheapest way to provide for surge capacity is to learn first aid. And keep some medical supplies available. Providing you are breaking no drug laws by keeping pain killers or other drugs around for those who weren’t prescribed them.
My wife works with veterinarians, who are (drum roll please) being signed up by the Homeland Security folks as ‘first responders’ in case of a major catastrophic increase in local care needs (e.g. terrorist attack). It makes sense. Just as those with a runny nose would be thrown out of the ER (making more room) in the even of a terrorist attack or major flu epidemic, the addition of people who know how to set bones, stitch wounds, look at xrays, administer medicine, etc would be a big surge capacity boon in times of need (of course the tendency to check to see if the nose was wet might get to be annoying). To say that a system that is running near capacity is thus incapable of handling a disaster is at best not looking at everything.
Just for James, I wonder if the study controlled for whether a city was encouraging illegal immigration by not checking immigration status for rendering services (such as hospital care) or not. Just asking.
Why is it that I don’t put it past Steve to be Pro “Socialized Medicine”.
Now I know he is a hard core LIBERAL.
For what it’s worth, I had a minor injury in Paris, France, a couple of years ago (stupidly walked into a door at the D’Orsay). I went to the emergency room in an ambulance, accompanied by two attendants, was glued together and sent on my way in less than a half-hour, by a number of people who spoke better English than my lousy French, all for free. That evening at dinner (delicious dinner) a Finnish woman told me that on her first night in Paris, before she started her new job with an EU entity, she was sick, and the hotel called a doctor, who made a house call. For Free.
The per capita expenditure of the French in 2003 was a bit more than half of the US. tables at
Sorry, apparently do not understand how to do links.
http://tinyurl.com/6phzp for the tables I mentioned above.
The thing about pregnancy is that it can be tremendously expensive, and there’s no way of knowing in advance whether you’re getting a $2000 pregnancy or a $200,000 pregnancy. Seems like the sort of thing a body would insure to me. Of course, that doesn’t solve the problem of how best to go about this, or the public health issues that are inevitably raised around prenatal care, but that’s beside my current point. Contraceptive failure must also be dealt with, but again, beside my point. The question of what, exactly, insurance is for is a good one, though, and in some ways I think really at the heart of the issue.